What causes Alzheimer’s Disease? Talk about a complex question! Even with research dating back to the early 1900s, scientists do not completely know the answer. There are many different answers out there: aging, genetics, viral infection, autoimmune disorders, etc. However, most scientists can agree on one thing – there is no single cause for Alzheimer’s Disease. Research suggests that a virus that causes herpes may be involved. So are herpes and Alzheimer’s disease related?
So, what is Alzheimer’s Disease?
Alzheimer’s Disease (AD) is a progressive disease with symptoms that include irreversible memory loss, cognitive decline, and an overall deterioration of everyday social function. From a medical perspective, AD is described by an overaccumulation of two proteins normally found in the brain, amyloid β plaques and protein tau tangles. When these proteins are over produced, or when they are improperly formed, they can lead to the death of brain cells called neurons. Even though the cause of AD is not fully known, multiple risk factors and comorbidities (two or more diseases at the same time) have been noted, such as cardiovascular disease, diabetes, and viral infections.
The Brain Game
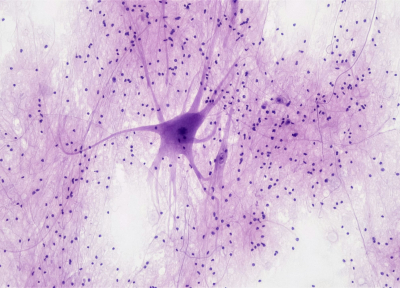
Your brain is a very powerful organ. It contains billions of neurons that form trillions of connections, allowing you to do basic things like walk, talk, eat, drink, sleep, and breathe, as well as process the world around you. Although your brain is highly protected, it is not immune to infection. Bacteria and viruses are both capable of infecting the brain, causing inflammation and damage to brain cells.
So how does the brain protect itself from infection? That is where its own personal army comes into play: the neuroimmune system. The neuroimmune system is made up of a variety of different cells that help to both maintain the brain during normal, healthy conditions as well as mount a defense when the brain is under attack from germs. There are two main players: astrocytes and microglia.
Astrocytes are star-shaped cells that primarily provide structure and support to neurons, while microglia are a type of cell that “eat” dead cells, cellular debris, and germs. Together, astrocytes and microglia work to ensure your brain is functioning at the highest level it can by protecting your sensitive and nonrenewable neuronal cells from foreign invasion. Neurodegenerative diseases can arise when one or both of these cell types start misbehaving, leading to either a poor immune response to infection or chronic inflammation.
In Alzheimer’s Disease, we know that microglia play a pivotal role. Their overactivation, or activation over a long period of time, can can cause excessive swelling in the brain and nervous system and a rapid increase in toxins, which leads to a loop of more activation, more inflammation, and worse symptoms.
Linking Herpes and Alzheimer’s Disease
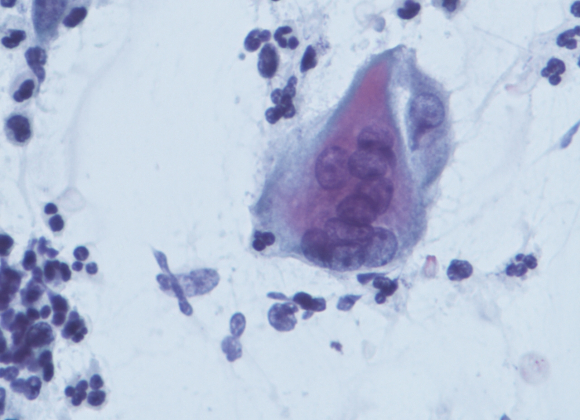
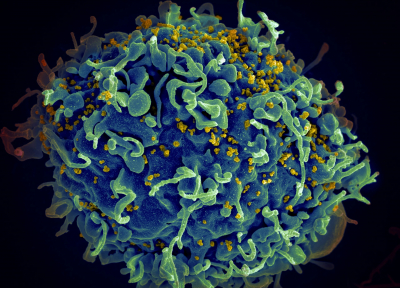
One common virus, herpes simplex virus type 1 or HSV-1, has been linked to multiple neurodegenerative diseases, including AD. HSV-1 is a virus that infects cells near mucosal membranes on your face and forms blisters (cold sores). Once it infects those skin cells, it has access to neurons and the nervous system. Eventually the virus goes latent in the neuron cell bodies, meaning it enters “incognito mode” and can go undetected by the cells of the immune system. Once HSV-1 reaches the brain, microglia are activated and mount a response to clear the infection, eventually forcing the virus back into its undetectable state. In AD, researchers suggest that once the microglia clear this initial HSV-1 infection, they remain at a highly activated state, leading to greater inflammation that potentially worsen AD.
Researchers like myself are trying to untangle the complicated web of factors that can cause AD. I am looking at what happens when HSV-1 infects the brain before someone has AD. Most research linking HSV-1 and AD is correlative in nature, meaning we know there is a relationship, but we don’t know if one causes the other. It becomes a classic chicken vs. egg conundrum of which came first, HSV-1 infection or AD? Our research seeks to answer this by studying what happens during HSV-1 infection before AD arises. Understanding the relationship between HSV-1 and AD, could allow researchers to create antiviral drugs that would keep the virus in its incognito mode to reduce the over activation of microglia that can cause neuroinflammation, potentially slowing down or preventing cognitive decline.
Ellen Fleming is earning her PhD in the Ocular Microbiome and Immunity Laboratory under Dr. Anthony St. Leger at the University of Pittsburgh.